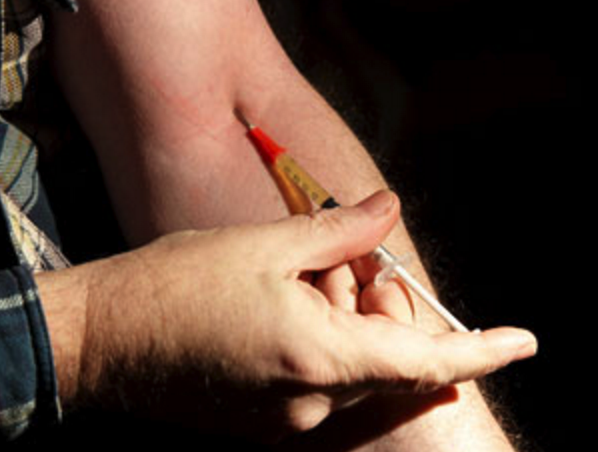
Infectious disease physicians are intimately familiar with injection drug use for the obvious reason that breaching the skin and injecting substances directly into the bloodstream is a path to paradise for most microorganism. Unfortunately for humans, that path to paradise is paved with infective endocarditis (infection of the heart valves), abscesses, infections of veins (septic thrombophlebitis), HIV, hepatitis C, and hepatitis B (not to mention anthrax, tetanus, and botulism). Injection drug use is the primary problem with infections following secondarily and unless the injection drug user stops or is able to learn how to inject more skillfully (with clean needles and skin antisepsis) recurrent infections will be the norm.
This weekend I took care of a thirty-something injection drug user who recently had Staphylococcus aureus ("staph"), a common organism that infects injection drug users, in the bloodstream resulting in destruction of two heart valves as well as an abscess in the aorta. This was treated with a long course of antibiotics followed by surgery that involved the use of prosthetic valves and repair of the aorta. The infection was cured for a while until injection drug use resumed and another bloodstream infection ensued with evidence of infection of all the prosthetic material put in place, a dire situation as bacteria form hardy biofilms on prosthetic material that are somewhat impervious to antibiotic therapy. This will be a difficult infection to control or cure and thoracic surgeons don't relish doing these types of repeat surgeries.
This scenario got me thinking about the phenomenon of injection drug use infections of heart valves and the special problems it poses. Because recurrence is the rule, certain rules applied to valve infections/replacements may not necessarily apply For example, using more durable mechanical heart valves in younger patients and bioprosthetic versions of bovine or pig origin in older patients who will not live long enough for the valve to need replacement. In one study, at 5 years less than half (46.7%) of injection drug users endocarditis patients are alive while over 70% of those that are not injection drug users are alive, arguing against the routine practice of using mechanical valves as a matter of routine in injection drug users.
I don't know what will happen with this particular patient but the important aspect of the case is understanding that unless the primary problem is corrected -- the injection drug use -- no level of aggressiveness in infection management will ultimately change the outcome.